تنزيل برنامج Format Factory أخر اصدار برابط مباشر مع الشرح

من خلال تحميل برنامج فورمات فاكتوري ، Format Factoryعربي للكمبيوتر مجانا والذي يطلق عليه ايضاً اسم مصنع الصيغ يستطيع المستخدم تحويل صيغ الوسائط المتعددة بسرعة كبيرة ويدعم البرنامج امكانية تحويل صيغ الفيديو وكذلك الصور والملفات الصوتية بكل سهولة كما يمكنه تقليل حجم تلك الملفات الى حجم اقل وبالتالى استهلاك مساحة أقل من القرص الصلب وتوفير النفقات وهذا ما يجعل التعامل معاها اسهل ايضاً وبشكل خاص فى عملية النقل من مكان الى اخر على الكمبيوتر او النسخ والنقل على الاقراص الخارجية .
نرشح لك : تحميل برنامج Truecaller أخر تحديثات 2022 مع الشرح
https://www.youtube.com/watch?v=o0ZLUKeduNU
تغيير صيغ الملفات وامكانية تشغيلها على الاجهزة الاخرى !
من خلال تغيير صيغ الملفات يمكن اختيار صيغ اخرى ليتمكن المستخدم من تشغيلها على الاجهزة الاخرى مثل الهواتف المحمولة او شاشات العرض الذكية والتلفزيون والشاشات التى تدعم اللمس وبالتالى امكانية استخدام وتشغيل مقاطع الفيديو الخاصة بك على اى جهاز من اجهزتك ودون اى عناء وعملية التحويل بأستخدام البرنامج تتم بسرعة كبيرة كما ان البرنامج مجاني تماماً وبالتالى يمكنك توفير النفقات والاستمتاع بأستخدام هذا البرنامج مجاناً لأنه احترافي بالفعل ويقدم برنامج Format Factory 2018 تجربة رائعة لمستخدميه فى تحويل الصيغ من عدة اتجاهات مثل السرعة والسهولة والامان والحفاظ على جودة الفيديو مع تقليل المساحة وتوافر الكثير من الادوات الاحترافيه التى تساعد المستخدمين على اخراج عمل احترافي بالنهاية ويأتى الاصدار الجديد من البرنامج كما اعتاد عليه المستخدمون سهل الاستخدام بواجهة مستخدم لما يتم تغييرها كثيراً لتظل سهلة وواضحة.

فورمات فاكتوري هو الافضل لتحويل صيغ الفيديو من صيغة لأخرى
- البساطه: بأختصار شديد لتلك النقطه فأن برنامج فورمات فاكتوري هو احد اسهل التطبيقات التى يمكن ان تتعامل معاها على جهاز الكمبيوتر لديك فى المطلق وذلك نظراً لوضوح واجهة المستخدم الخاصة بالبرنامج بالاضافة الى سهولة العمل عليه بشكل كامل وتحويل من اى صيغة يدعمها البرنامج الى الصيغة الاخرى.
- تصغير الحجم: من خلال استخدامك لهذا البرنامج تستطيع تحويل مقاطع الفيديو الصغيرة الحجم او شرائط الفيديو الطويلة والتى تمتد الى ساعات طويلة وكذلك الصوتيات والصور وتقليل حجم تلك الملفات الى اصغر حجم ممكن دون المساس بجودة الفيديو وهذا كله بالطبع يعود نسبياً على المستخدمين بالنفع من ناحية من عدة اتجاهات اهمها توفير المساحة التى يتم استهلاكها على الهارد ديسك واستخدامها لأضافة المزيد من الملفات وكذلك سهولة نقل ونسخ تلك الملفات من مكان لأخر.
- تحويل الفيديو: الميزة الاساسية فى هذا العملاق المجاني هى امكانية تحويل صيغ الفيديو من صيغة لأخرى بثبات مع الحفاظ على جودة الفيديو كما هى بل واصلاح المشكلات ان وجدت مع امكانية تحويل جميع صيغ الفيديو الشعبية الى MP4/3GP/MPG/AVI/WMV/FLV/SWF بل ويسمح البرنامج بأمكانية تحويل الفيديو الى صوت Mp3 او صيغ اخرى من التى يدعمها البرنامج وهى متعددة وكثيرة جداً.
تحويل صيغ الفيديو باستخدام فورمات فاكتوري
- دعم التحويل لصيغة Mp4 للهواتف: يدعم البرنامج الفيديو بصيغة Mp4 والذى يعمل على اجهزة الهواتف المختلفة مثل الايفون والايباد والبلاك بيري واجهزة PSP ايضاً وبالتالى تستطيع تشغيل مقاطع الفيديو الخاصة بك على الهاتف بجودة عالية دون الحاجة الى تحويلها لصيغ اخرى.
- العلامات المائية: يمكنك اضافة علامة مائيه على مقاطع الفيديو اثناء تحويلها مع صيغة RMVB ومقاطع الفيديو وبهذا يمكنك اضافة اى من الشعارات على مقاطع الفيديو.
- النسخ على الاقراص المدمجة: يمكنك نسخ مقاطع الفيديو والصوتيات وكذلك الصور مباشرة على اسطوانة مدمجة سواء كانت CD او DVD بسهولة من خلال البرنامج حتى انه يمكنك نسخ اسطوانات صوتيه لتعمل مباشرة على مشغل الاسطوانات لديك بالسيارة او على جهاز الكمبيوتر كأسطوانة صوت او فيديو لتتمكن من عرضها على المشغل اسطوانات الفيديو سي دى (VCD) بسهولة.
- تعدد اللغات: البرنامج متوفر بعشرات اللغات المختلفة يمكنك استخدام برنامج مصنع الصيغ 2018 باللغة التى تفضلها من اللغات المتوفره بالبرنامج والتى من اهمها اللغة الانجليزية والفرنسية والايطالية والعربية والاسبانية ولغات اخرى كثيرة وتغيير لغة البرنامج من لغة الى اخرى سهل للغاية على اى شخص من خلال الادوات فى البرنامج.
- المظهر: يستطيع المستخدم تخصيص مظهر واجهة البرنامج ولونها حسب تفضيله من 7 الوان مختلفة موجودة للواجهة لتتماشى مع ذوق المستخدم منها الابيض والاخضر والازرق والاسود والبينك.
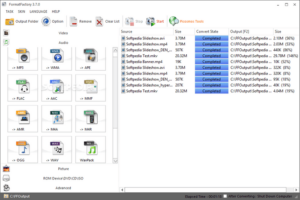
مراجعة لأخر اصدار من برنامج فورمات فاكتوري 2018
اعتاد على استخدام هذا البرنامج ملايين المستخدمين ونحن فى موقع برامج جديدة نفضل استخدام هذا البرنامج خاصة انه مجاني منذ انطلاق الاصدار الاول منه وحتى انطلاق Format Factory 2018 الاصدار الحديث بالاضافة لأنه سهل رغم توافر العديد من الادوات الاحترافيه به وامكانية تخصيص الواجهة الخاصة بالبرنامج وكذلك اللغة ودعم العديد من صيغ الوسائط المتعددة بما فيها جميع الصيغ الشعبية وهذا ما يتوفر بالاصدار الجديد مع مميزات اضافية.
معلومات ملف تحميل فورمات فاكتوري 2018 اخر اصدار
الحجم: 50 ميجا بايت
نظام التشغيل: ويندوز
اسم البرنامج: Format Factory 2018
المطور: Free Time
الترخيص: مجانا
نرشح لك : تنزيل برنامج zoom للاندرويد والايفون أخر تحديث 2022 مع الشرح




